Ventricular Assist Devices (VADs) are advanced mechanical pumps used to support heart function and blood flow in people with severe heart failure. They help the heart pump blood more effectively when it is too weak to meet the body’s needs. VADs have become an important life-saving therapy for patients awaiting heart transplantation or those who are not candidates for transplant.
What Is a Ventricular Assist Device?
A Ventricular Assist Device is a mechanical pump that is surgically implanted to help one or both ventricles of the heart pump blood. The device takes over part or most of the heart’s pumping function, allowing the weakened heart to rest and recover or supporting the patient long-term.
VADs do not replace the heart but assist it in circulating blood throughout the body.
Why Are VADs Needed?
VADs are recommended for patients with advanced (end-stage) heart failure who experience:
- Severe shortness of breath
- Extreme fatigue
- Fluid retention
- Frequent hospitalizations
- Poor response to medications
They are used when standard treatments such as medicines or cardiac devices (pacemakers, ICDs) are no longer effective.
Types of Ventricular Assist Devices
- Left Ventricular Assist Device (LVAD): Supports the left ventricle, most commonly used type, pumps blood from the left ventricle to the aorta.
- Right Ventricular Assist Device (RVAD): Supports the right ventricle, often used temporarily after heart surgery or transplant.
- Biventricular Assist Device (BiVAD): Supports both ventricles, used in severe, two-sided heart failure.
Purposes of VAD Therapy
- Bridge to Transplant: Keeps patients stable while waiting for a heart transplant.
- Destination Therapy: Long-term treatment for patients who are not candidates for transplant.
- Bridge to Recovery: Supports the heart temporarily while it heals and regains function.
- Bridge to Decision: Used when doctors need time to determine the best long-term treatment.
How Does a VAD Work?
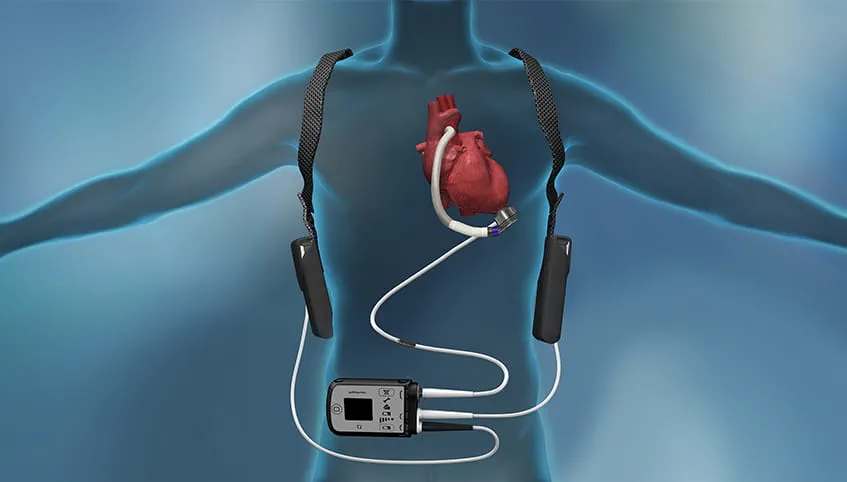
A VAD system has several components:
- Pump: Implanted inside the chest or abdomen.
- Cannulas: Tubes that move blood in and out of the pump.
- Driveline: A cable that exits the body through the skin.
- Controller: Regulates pump function.
- Power source: Batteries or AC power.
The device runs continuously and requires constant power.
Implantation Surgery
VAD implantation is a major surgical procedure performed under general anesthesia.
Procedure Overview:
- Chest is opened (or minimally invasive approach in select cases).
- Pump is connected to the heart and aorta.
- Driveline is tunneled through the skin.
- Device function is tested.
- Chest is closed.
Surgery typically lasts 4–6 hours.
Recovery After VAD Implantation
Hospital Recovery
ICU stay: several days
Hospital stay: 2–4 weeks
Physical rehabilitation begins early.
Home Care
Patients and caregivers receive training on:
- Battery and controller management.
- Driveline care and infection prevention.
- Recognizing device alarms.
- Emergency procedures.
Living With a Ventricular Assist Device
Most patients experience:
- Improved energy levels.
- Reduced breathlessness.
- Better exercise tolerance.
- Improved quality of life.
Lifestyle adjustments include:
- Daily device checks.
- Avoiding water immersion (no swimming).
- Careful skin hygiene.
- Regular follow-ups.
Risks and Complications
While life-saving, VADs carry potential risks:
- Infection (especially at driveline site).
- Blood clots.
- Stroke.
- Bleeding.
- Device malfunction.
Strict medication use (blood thinners) and hygiene reduce these risks.
Medications After VAD Implantation
Patients usually require:
- Blood thinners (anticoagulants).
- Antiplatelet drugs.
- Heart failure medications.
- Antibiotics (if needed).
Regular blood tests are essential.
Who Is a Candidate for VADs?
VADs may be suitable for patients who:
- Have end-stage heart failure.
- Are not responding to medical therapy.
- Are awaiting heart transplant.
- Have acceptable organ function.
- Can manage device care with support.
Each patient undergoes detailed evaluation before implantation.
Life Expectancy and Outcomes
Advances in VAD technology have significantly improved survival. Many patients live several years with good quality of life on VAD support. Outcomes depend on overall health, complications, and adherence to care instructions.
When to Contact Your Doctor
Seek immediate medical attention if:
- Device alarms sound repeatedly.
- Fever or signs of infection appear.
- Sudden weakness or speech problems occur.
- Unusual bleeding develops.
- Shortness of breath worsens.
